Explore the Practice Resource Centre

EXPLORE THE PRACTICE RESOURCE CENTRE – we are pleased to share the new PRC promotional video. In just over two minutes, we highlight the benefits of the site for seasoned practitioners and those just starting their career, how to easily submit ideas and resources, how to create a custom reading list, and much more.
Glaucoma OCT Interpretation: 101
Glaucoma OCT Interpretation is an online, Section 3 accredited course available at EyeCarePD.com. A game-based approach is applied to learning OCT interpretation. This course covers commonly encountered OCT presentations of glaucoma as seen on standard optic nerve head and retinal nerve fiber layer scan protocols with the purpose of improving interpretation skills using perceptual learning strategies.
Getting started is easy:
- Using the Google Chrome browser, navigate to https://eyecarepd.com/catalog/glaucoma-group/
- Select Glaucoma OCT Interpretation 101 (COS Accredited) and add the product to the cart
- At checkout, use the coupon code ECPDCOSGLAUCOMA to set the price to 0.
- Your course is now available under My Courses at the top of the screen.
Learning Objectives:
- Identify segmentation errors and their role in OCT scan interpretation
- Utilize varying sections of the OCT report including tabular data, sector analysis and graphical displays
- Interact with expert interpretation in order to compare their findings in selected cases
Accreditation
This activity is an Accredited Self-Assessment Program (Section 3) as defined by the Maintenance of Certification program of the Royal College of Physicians and Surgeons of Canada. This web-based lesson was approved by the COS on October 23rd, 2020 and expires October 2023. Remember to visit MAINPORT to record your learning and outcomes. You may claim a maximum of 1 hour (credits are automatically calculated).
This activity was co-developed with EyeCarePD and the Canadian Ophthalmological Society (COS) and was planned to achieve scientific integrity, objectivity and balance.
Access Details
To participate in this course visit https://eyecarepd.com/catalog/glaucoma-group/


EyeNovation Webinar: The Evolving Landscape of CAIRS – Recording

Did you miss the webinar? Not to worry, a recording is available for you below!
Our EyeNovation webinar featured Dr. Awwad, who presented on The evolving landscape of CAIRS.
This session explored the latest developments in CAIRS, including evolving surgical techniques, preparation methods, and clinical outcomes, offering valuable, practice-oriented insights for ophthalmologists and trainees.

Dr. Shady Awwad is Professor of Ophthalmology and Head of the Cornea & Refractive Surgery Division at the American University of Beirut Medical Center, where he also founded the Refractive Surgery Fellowship Program. He is internationally recognized for his expertise in refractive and keratoconus surgery and has authored more than 130 peer-reviewed publications.
Dr. Awwad serves as Associate Editor of the Journal of Refractive Surgery and sits on the Editorial Board of the American Journal of Ophthalmology. His work has earned numerous international distinctions, including the George Waring Medal for Editorial Excellence and the AAO Achievement Award. He has also contributed innovative analytical tools and formulas to major ophthalmic platforms and holds patents in artificial intelligence and computer vision related to ophthalmic surgery.
Learning Objectives
By the end of this session, participants will be able to:
- Introduction to CAIRS, their outcomes and their mechanism of action
- Insights into the changing trends in CAIRS preparation, insertion, and surgical techniques.
Keratoprosthesis: Best Practices – Preoperative, Operative and Postoperative
University of Toronto and Wills Eye Hospital are proud to present the next installment of the Cornea Surgical Video Learning Series

Date: Thursday, May 14th, 2026
Time: 1930 – 2100 PM EDT
Co-moderated by Professors Sadeer Hannush (Wills Eye Hospital) and Allan Slomovic (University of Toronto).
Keynote Lecturer
Mona Dagher MD, FRCSC
Professor, University of Montreal
Head of Ophthalmology, Centre Hospitalier de l’Université de Montréal (CHUM)
Guest Panellists
Neera Singal MD, FRCSC and Clara Chan MD, FRCSC (University of Toronto)
Marisa Schoen MD & Zeba Syed MD (Wills Eye Hospital)
Surgery Case Presentations
Maria Rizk MD, FRCSC (Université de Montréal)
Betul Bayraktutar MD, DO (Wills Eye Hospital)
You are invited to a Zoom webinar. You must register in order to join and receive your CPD.
https://us02web.zoom.us/webinar/register/WN_CjpTHmDnRs-z1kvSbjvEGA#
After registering, you will receive a confirmation email containing information about joining the webinar.
The evening will as usual be recorded and placed online for viewing.
If you would like to view prior sessions in the series, please visit:
https://ophthalmology.utoronto.ca/subspecialty-rounds
CME credits are available for the following:
· Royal College Maintenance of Certification Section 1: 1.5 hours (1.5 Section 1 hours per session)
· American Medical Association Category 1: 1.5 credits (1.5 Category 1 credits per session)
· European Union for Medical Specialists UEMS-EACCME®: 1.5 credits (1.5 ECMEC credits per session)
Ergonomics: Journal Articles & Editorials
- Bolis M, Garg A, Chan B. Real-time postural feedback to optimize ergonomics and musculoskeletal health in ophthalmology residents: a Canadian pilot quality improvement study. Cureus 2025;17(7):e88736. DOI: 10.7759/cureus.88736 https://pubmed.ncbi.nlm.nih.gov/40717881/
- Buchmann W, Fortineau E, Ribaute E, Brezin A. [Musculoskeletal problems in ophthalmology, risk factors and solutions: case studies from two French practices]. Journal Français d’Ophtalmologie 2025;48(7):104578. DOI: 10.1016/j.jfo.2025.104578 https://pubmed.ncbi.nlm.nih.gov/40669315/
- Ismail MM, Fayyadh RA, Hassanein DH, et al. Prevalence and risk factors of musculoskeletal pain among pediatric ophthalmologists and strabismologists in the Middle East: a cross-sectional study. Journal of Pediatric Ophthalmology and Strabismus 2026;63(1):65-73. DOI: 10.3928/01913913-20250701-01 https://pubmed.ncbi.nlm.nih.gov/40736052/
- Kaur H, Xie JS, Lusterio A, et al. A scoping review of ergonomics in ophthalmology: working in pain. American Journal of Ophthalmology 2026;282:433-57. DOI: 10.1016/j.ajo.2025.11.005 https://pubmed.ncbi.nlm.nih.gov/41242593/
- Nishant P, Singh A, Morya AK, et al. Manual small incision cataract surgery: an ergonomic solution to tackle cataract backlog and challenging situations. World Journal of Methodology 2025;15(4):104529. DOI: 10.5662/wjm.v15.i4.104529 https://pubmed.ncbi.nlm.nih.gov/40900862/
- Sather RN, 3rd, Moon JY, Romano F, et al. The ergonomic evaluation of attendings and trainees across the vitreoretinal service as measured by a wearable device. Ophthalmic Surgery, Lasers and Imaging Retina 2025;56(2):80-5. DOI: 10.3928/23258160-20240906-01 https://pubmed.ncbi.nlm.nih.gov/39311565/
- Sinha S, Nishant P, Sinha RK. Experience and challenges in intraocular surgery in patients with kyphosis: a cross-sectional survey among practicing ophthalmologists. Cureus 2025;17(8):e89490. DOI: 10.7759/cureus.89490 https://pubmed.ncbi.nlm.nih.gov/40918920/
- Tanya SM, Kulbay M, Kherani A, et al. Ergonomic impact of electronic medical records on Canadian eye care providers: results from the Canadian ophthalmic practitioners ergonomics survey. Canadian Journal of Ophthalmology 2026. DOI: 10.1016/j.jcjo.2026.01.008 https://pubmed.ncbi.nlm.nih.gov/41620202/
- Xie JS, Kaur H, Lusterio A, et al. A scoping review of ergonomics in ophthalmology: working smarter. American Journal of Ophthalmology 2026;281:249-69. DOI: 10.1016/j.ajo.2025.08.053 https://pubmed.ncbi.nlm.nih.gov/40889624/
- Aloqab A, Alturkistany W, Ali HMN. The relationship between surgical loupes usage, workplace ergonomics, and musculoskeletal disorders among Saudi ophthalmologists. Saudi Journal of Ophthalmology. 2024; 3;39(2):166-173. DOI: 10.4103/sjopt.sjopt_276_23. https://pubmed.ncbi.nlm.nih.gov/40642356/
- Morrison AK, Kumar S, Amin A, Urban M, Kleinman B. An ergonomic risk assessment of ophthalmology residents using the Rapid Entire Body Assessment (REBA) scale. Cureus 2024;16(2):e53698. DOI: 10.7759/cureus.53698. https://pubmed.ncbi.nlm.nih.gov/38455825/
- Kamei M, Suzuki H, Terayama H, et al. Ergonomic benefit using heads-up display compared to conventional surgical microscope in Japanese ophthalmologists. PLoS One 2024;19(5):e0297461. DOI: 10.1371/journal.pone.0297461. https://pubmed.ncbi.nlm.nih.gov/38776346/
- Barrios EL, Polcz VE, Hensley SE, et al. A narrative review of ergonomic problems, principles, and potential solutions in surgical operations. Surgery 2023;174(2):214-221. DOI: 10.1016/j.surg.2023.04.003. https://pubmed.ncbi.nlm.nih.gov/37202309/
- Fouzdar Jain S, Akhter S, Ishihara R, Siddicky S, High R, Suh DW. The prevalence of work-related musculoskeletal disease among pediatric ophthalmologists. Clinical Ophthalmology 2022;16:833-840. DOI: 10.2147/OPTH.S343155. https://pubmed.ncbi.nlm.nih.gov/35330751/
- Cerier E, Hu A, Goldring A, Rho M, Kulkarni SA. Ergonomics Workshop Improves Musculoskeletal Symptoms in General Surgery Residents. Journal of Surgical Research 2022;280:567-574. DOI: 10.1016/j.jss.2022.06.014.https://pubmed.ncbi.nlm.nih.gov/35787315/
- Albanesi B, Piredda M, Bravi M, et al. Interventions to prevent and reduce work-related musculoskeletal injuries and pain among healthcare professionals. A comprehensive systematic review of the literature. Journal of Safety Research 2022;82:124-143. DOI: 10.1016/j.jsr.2022.05.004. https://pubmed.ncbi.nlm.nih.gov/36031239/
- Aaron KA, Vaughan J, Gupta R, et al.The risk of ergonomic injury across surgical specialties. PLoS One 2021;16(2):e0244868. DOI: 10.1371/journal.pone.0244868. https://pubmed.ncbi.nlm.nih.gov/33561117/
- Schechet SA, DeVience E, DeVience S, Shukla S, Kaleem M. Survey of musculoskeletal disorders among US ophthalmologists. Digital Journal of Ophthalmology 2021;26(4):36-45. DOI: 10.5693/djo.01.2020.02.001. https://pubmed.ncbi.nlm.nih.gov/33867881/
- Koshy K, Syed H, Luckiewicz A, Alsoof D, Koshy G, Harry L. Interventions to improve ergonomics in the operating theatre: A systematic review of ergonomics training and intra-operative microbreaks. Annals of Medicine & Surgery (Lond) 2020;55:135-142. DOI: 10.1016/j.amsu.2020.02.008. https://pubmed.ncbi.nlm.nih.gov/32477512/
- Betsch D, Gjerde H, Lewis D, Tresidder R, Gupta RR. Ergonomics in the operating room: it doesn’t hurt to think about it, but it may hurt not to! Canadian Journal of Ophthalmology 2020;55(3 Suppl 1):17-21. DOI: 10.1016/j.jcjo.2020.04.004. https://pubmed.ncbi.nlm.nih.gov/32448408/
- Weng CY, Hariprasad SM, Leiderman YI. Ergonomics in retina. Ophthalmic Surgery, Lasers and Imaging Retina 2019;50(9):537-542. DOI: 10.3928/23258160-20190905-01. https://pubmed.ncbi.nlm.nih.gov/31589750/
- Epstein S, Tran BN, Capone AC, et al. The current state of surgical ergonomics education in U.S. surgical training: a survey study. Annals of Surgery 2019;269(4):778-784. DOI: 10.1097/SLA.0000000000002592. https://pubmed.ncbi.nlm.nih.gov/29381528/
- Diaconita V, Uhlman K, Mao A, Mather R. Survey of occupational musculoskeletal pain and injury in Canadian ophthalmology. Canadian Journal of Ophthalmology 2019;54(3):314-322. DOI: 10.1016/j.jcjo.2018.06.021. https://pubmed.ncbi.nlm.nih.gov/31109470/
- Bonafede L, Kazmierczak L, Siddicky SF, Gunton KB. Ergonomics in strabismus surgery. Current Opinion in Ophthalmology 2019;30(5):331-336. DOI: 10.1097/ICU.0000000000000594. https://pubmed.ncbi.nlm.nih.gov/31313751/
- Ratzlaff TD, Diesbourg TL, McAllister MJ, von Hacht M, Brissette AR, Bona MD. Evaluating the efficacy of an educational ergonomics module for improving slit lamp positioning in ophthalmology residents. Canadian Journal of Ophthalmology 2019;54(2):159-163. DOI: 10.1016/j.jcjo.2018.05.016. https://pubmed.ncbi.nlm.nih.gov/30975337/
- Kaup S, Shivalli S, Kulkarni U, Arunachalam C. Ergonomic practices and musculoskeletal disorders among ophthalmologists in India: An online appraisal. European Journal of Ophthalmology 2020;30(1):196-200. DOI: 10.1177/1120672118815107. https://pubmed.ncbi.nlm.nih.gov/30474398/
- Venkatesh R, Kumar S. Back pain in ophthalmology: National survey of Indian ophthalmologists. Indian Journal of Ophthalmology 2017;65(8):678-682. DOI: 10.4103/ijo.IJO_344_17. https://pubmed.ncbi.nlm.nih.gov/28820152/
- Shaw C, Bourkiza R, Wickham L, McCarthy I, McKechnie C. Mechanical exposure of ophthalmic surgeons: a quantitative ergonomic evaluation of indirect ophthalmoscopy and slit-lamp biomicroscopy. Canadian Journal of Ophthalmology 2017;52(3):302-307. DOI: 10.1016/j.jcjo.2016.09.011. https://pubmed.ncbi.nlm.nih.gov/28576213/
- 2Honavar SG. Head up, heels down, posture perfect: Ergonomics for an ophthalmologist. Indian Journal of Ophthalmology 2017;65(8):647-650. DOI: 10.4103/ijo.IJO_711_17. https://pubmed.ncbi.nlm.nih.gov/28820146/
- Sivak-Callcott JA, Mancinelli CA, Nimbarte AD. Cervical occupational hazards in ophthalmic plastic surgery. Current Opinion in Ophthalmology 2015;26(5):392-8. DOI: 10.1097/ICU.0000000000000182. https://pubmed.ncbi.nlm.nih.gov/26247136/
- Alrashed WA. Ergonomics and work-related musculoskeletal disorders in ophthalmic practice. Imam Journal of Applied Sciences 2016;1(2):48-63. DOI: 10.4103/ijas.ijas_24_16. https://journals.lww.com/ijas/fulltext/2016/01020/ergonomics_and_work_related_musculoskeletal.2.aspx
- Hyer JN, Lee RM, Chowdhury HR, Smith HB, Dhital A, Khandwala M. National survey of back & neck pain amongst consultant ophthalmologists in the United Kingdom. International Ophthalmology 2015;35(6):769-775. DOI: 10.1007/s10792-015-0036-z. https://pubmed.ncbi.nlm.nih.gov/25609503/
- Herzog NV, Beharic RV, Beharic A, Buchmeister B. Ergonomic analysis and simulation in department of ophthalmology. Procedia Manufacturing 2015;3:128-135. DOI: 10.1016/j.promfg.2015.07.117. https://www.researchgate.net/publication/283960343_Ergonomic_Analysis_and_Simulation_in_Department_of_Ophthalmology
- Fethke NB, Schall MC, Determan EM, Kitzmann AS. Neck and shoulder muscle activity among ophthalmologists during routine clinical examinations. International Journal of Industrial Ergonomics 2015;49:53-59. DOI: 10.1016/j.ergon.2015.06.001. https://www.sciencedirect.com/science/article/abs/pii/S0169814115300019
- Hedge A, James T. Detrimental Effects of an electronic health records system on musculoskeletal symptoms among health professionals. Proceedings of the Human Factors and Ergonomics Society Annual Meeting 2014;58(1):773-777. DOI: 10.1177/1541931214581141. https://www.researchgate.net/publication/271722221_Detrimental_Effects_of_an_Electronic_Health_Records_System_on_Musculoskeletal_Symptoms_among_Health_Professionals#:~:text=Exposure%20to%20blood%20and%20body,of%20health%20practitioners%20surveyed%20reported
- Mehta S, Hubbard GB, 3rd. Avoiding neck strain in vitreoretinal surgery: an ergonomic approach to indirect ophthalmoscopy and laser photocoagulation. Retina 2013;33(2):439-41. DOI: 10.1097/IAE.0b013e318276cbca. https://pubmed.ncbi.nlm.nih.gov/23190927/
- Dorion D, Darveau S. Do micropauses prevent surgeon’s fatigue and loss of accuracy associated with prolonged surgery? An experimental prospective study. Annals of Surgery 2013;257(2):256-9. DOI: 10.1097/SLA.0b013e31825efe87. https://pubmed.ncbi.nlm.nih.gov/22824853/
- Marx JL. Ergonomics: back to the future. Ophthalmology 2012;119(2):211-2. DOI: 10.1016/j.ophtha.2011.09.001. https://pubmed.ncbi.nlm.nih.gov/22305308/
- Kitzmann AS, Fethke NB, Baratz KH, Zimmerman MB, Hackbarth DJ, Gehrs KM. A survey study of musculoskeletal disorders among eye care physicians compared with family medicine physicians. Ophthalmology 2012;119(2):213-20. DOI: 10.1016/j.ophtha.2011.06.034. https://pubmed.ncbi.nlm.nih.gov/21925736/
- Theou O, Soon Z, Filek S, et al. Changing the sheets: a new system to reduce strain during patient repositioning. Nursing Research 2011;60(5):302-8. DOI: 10.1097/NNR.0b013e318225b8aa. https://pubmed.ncbi.nlm.nih.gov/21873921/
- Sivak-Callcott JA, Diaz SR, Ducatman AM, Rosen CL, Nimbarte AD, Sedgeman JA. A survey study of occupational pain and injury in ophthalmic plastic surgeons. Ophthalmic Plastic & Reconstructive Surgery 2011;27(1):28-32. DOI: 10.1097/IOP.0b013e3181e99cc8. https://pubmed.ncbi.nlm.nih.gov/20859236/
- Dhimitri KC, McGwin G Jr., McNeal SF, et al. Symptoms of musculoskeletal disorders in ophthalmologists. American Journal of Ophthalmology 2005;139(1):179-81. DOI: 10.1016/j.ajo.2004.06.091. https://pubmed.ncbi.nlm.nih.gov/15652844/
- Piccoli B, Committee IS. A critical appraisal of current knowledge and future directions of ergophthalmology: consensus document of the ICOH Committee on ‘Work and Vision’. Ergonomics 2003;46(4):384-406. DOI: 10.1080/0014013031000067473. https://pubmed.ncbi.nlm.nih.gov/12637175/
- Wallace RB, 3rd. The 45 degree tilt: improvement in surgical ergonomics. Journal of Cataract & Refractive Surgery 1999;25(2):174-6. DOI: 10.1016/s0886-3350(99)80122-9. https://pubmed.ncbi.nlm.nih.gov/9951660/
- Chatterjee A, Ryan WG, Rosen ES. Back pain in ophthalmologists. Eye (Lond) 1994;8 ( Pt 4):473-4. DOI: 10.1038/eye.1994.112. https://pubmed.ncbi.nlm.nih.gov/7821477/
EyeNovation Webinar: Herpes Simplex Keratitis – Recording

📅 Wednesday, March 25
⏰ 7:00–8:00 p.m. ET
Did you miss the webinar? Not to worry, a recording is available for you below!
We are pleased to invite you to our next EyeNovation webinar, “Herpes Simplex Keratitis,” presented by Dr. Sadeer B. Hannush, Professor of Ophthalmology at Thomas Jefferson University and Attending Surgeon on the Cornea Service at Wills Eye Hospital.
This session will provide a practical, clinically focused review of herpes simplex keratitis (HSK), addressing its varied presentations, impact on the anterior segment, and considerations for both medical and surgical management.
Learning Objectives
By the end of this session, participants will be able to:
- Differentiate and treat infectious versus immunologic forms of herpes simplex keratitis
- Describe the effects of HSK on the various layers of the anterior segment
- Discuss surgical management options for herpetic corneal scarring
2026 Paul Stringer Clinical Day in Ophthalmology, From Basics to Breakthroughs: Navigating the Spectrum of Cataract Surgery
McMaster University is excited to announce that registration is now open for the 2026 Paul Stringer Clinical Day in Ophthalmology – From Basics to Breakthroughs: Navigating the Spectrum of Cataract Surgery.
At the end of this activity, participants will be able to:
- Evaluate emerging innovations, technologies, and practice efficiencies in cataract surgery to inform evidence-based clinical decision-making.
- Apply refractive cataract surgery principles to optimize patient counseling, intraocular lens selection, and management of postoperative refractive outcomes.
- Adapt surgical strategies for complex cataracts and ocular comorbidities to enhance patient safety and clinical outcomes.
Date: Sunday, June 7, 2026
Time: 07:00–16:40
Location: Pillar and Post, 48 John Street West, Niagara-on-the-Lake, ON
Presented by McMaster University, Hamilton Regional Eye Institute, in Association with the Dr. Paul Stringer Memorial Lectureship
Early Bird ends May 3, 2026
Conference website: https://cpd.healthsci.mcmaster.ca/programs/ophthalmology-2026/
An agenda is available to view below:
World Uveitis Day

The Qatar Society of Ophthalmology and the Saudi Uveitis Group have recently launched the World Uveitis Day website.
The World Uveitis Day (WUD) was founded through the work of the Qatar Society of Ophthalmology and the Saudi Uveitis Group, under the leadership of the International Ocular Inflammation Society (IOIS), and major partnerships with the International Uveitis Study Group (IUSG), the Middle East & Africa Ophthalmology Uveitis Society (MEACO-US), and the Foster Ocular Immunology Society (FOIS). Key global uveitis experts and leaders have supported this initiative. Everyone is united to promote early detection of uveitis and its evidence-based care, to help patients and practitioners, and to prevent uveitis-related ocular complications and blindness.
The World Uveitis Day site has been created to make it easier to access reliable trustworthy information, and to raise awareness among people around the world about sight-threatening uveitis and ocular inflammatory diseases. On our website, patients, family members, care givers, and practitioners will be able to learn more about uveitis, treatments, and care options and identify and discover opportunities for uveitis disease knowledge on different levels.
The inaugural celebration of the World Uveitis Day will take place on April 10, 2026, in Doha, Qatar, where the initial concept first emerged. It will occur in association with the Second Qatar Uveitis Seminar to be held on April 11, 2026.
The OR Microscope – The Danger Zone
By Yusuf Ahmed, Mostafa Bondok, Patrick Gooi, and R. Rishi Gupta
The Surgical Chair
Ergonomic positioning in the OR begins with the surgical chair. Key features to consider include adjustable height (manual or electric), vertically adjustable lumbar support with horizontal adjustability when available, and a locking mechanism that provides stability. Features of commonly used chairs are provided in the images below.
The locking mechanism, when engaged, stabilizes the surgeon and improves fine motor control by allowing relaxation of the core and large stabilizing muscles. However, this same feature can “trap” the surgeon in a suboptimal position. Once alignment is achieved and the chair locked, it is important to recognize that periodic unlocking and micro-adjustments may be necessary as the case progresses and patient positioning shifts.

Optimize and Renew Your Form
Before the case begins, a brief “form check” is advisable. Relax your body, keep your neck neutral, stack your joints, and drop your shoulders down and back. Your back should be supported by the chair’s lumbar support, and your weight evenly distributed along the seat. Position arms and legs in a comfortable, symmetric posture, with pedals at a distance that doesn’t force reaching forward or backward. Finally, aim for hips slightly higher than knees (i.e., just over 90 degrees).
Poor ergonomic habits in the OR rarely reflect neglect. More often, they arise from cognitive load, time pressure, or fatigue. Surgeons may begin a case with excellent alignment, only to find that concentration, difficult anatomy, or prolonged duration gradually erode posture. When possible, distributing complex cases across the surgical schedule may reduce cumulative musculoskeletal strain in addition to cognitive fatigue.
The OR Microscope: A Static Trap
The OR microscope introduces a unique ergonomic challenge. Once the eyes are engaged in the oculars, the body tends to become fixed in position. If alignment is non-optimal, the surgeon may remain locked in a static, non-neutral posture for extended periods. Traditional advice to “sit up straight” is incorrect. Sustaining a rigid, upright posture increases muscular effort and often leads to compensatory strain. A more effective approach is to assess where the eyes would naturally fall if the body were completely relaxed. Any sensation of effort required to maintain ocular alignment should be treated as a signal that adjustments to the microscope, chair, and/or patient positioning should be made.
Three-Dimensional Alignment: OR microscope ergonomics can be conceptualized along three axes:
X-axis alignment – refers to left–right positioning. If the microscope is not centred relative to the surgeon, subtle lateral leaning or trunk side-bending occurs. Even small asymmetries can lead to uneven loading of paraspinal muscles and facet joints over time.

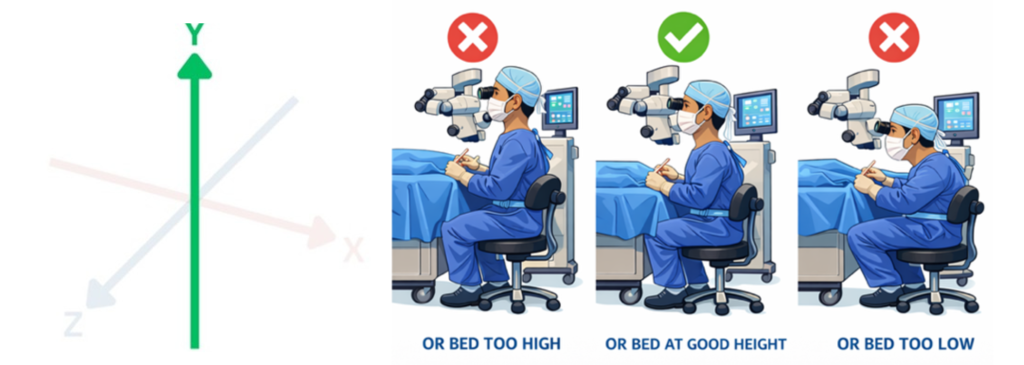
Y-axis alignment – reflects vertical positioning relative to the patient and surgical bed. When seated too low, surgeons compensate with cervical extension, increasing load on posterior cervical elements and paraspinal musculature. When seated too high, forward trunk and neck flexion predominate, increasing anterior cervical disc pressure, upper trapezius strain, and lumbar loading.
Z-axis alignment – refers to forward–backward positioning. Physical constraints imposed by chairs and pedals may prevent surgeons from positioning themselves close enough to the operative field, encouraging forward leaning. This increases lumbar disc pressure and thoracic flexion, often accompanied by compensatory cervical extension. Positioning the patient’s head closer to the edge of the headrest, when safely tolerated, can help reduce the need to reach forward.




